Merkel cell carcinoma (MCC) is a rare, aggressive skin cancer that demands prompt diagnosis and treatment. Though uncommon – with roughly 3,000 new cases diagnosed in the U.S. annually – its incidence has quadrupled in recent decades, likely due to improved testing and an aging population with cumulative sun exposure. This article provides a clear, concise guide to understanding MCC, from its symptoms and causes to treatment options and prevention.
Understanding the Disease
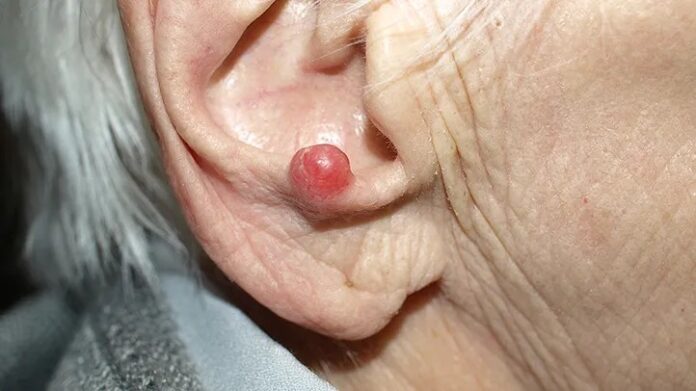
MCC typically presents as a firm, painless, pink, red, or purple bump on sun-exposed areas like the face, head, or neck. The bump grows rapidly, often in weeks to months, and may bleed. Because its appearance can mimic other skin conditions (bug bites, cysts, sores), early detection relies on recognizing speed of growth as a critical warning sign. The cancer can metastasize – spreading to lungs, brain, or bones – making early intervention crucial.
Why this matters: Unlike slower-growing skin cancers, MCC’s aggressiveness means delayed treatment can significantly worsen outcomes. The rise in cases suggests a need for greater public awareness and vigilance.
Causes and Risk Factors
While the exact cause remains unclear, research points to the Merkel cell polyomavirus as a potential trigger in some cases. However, the virus is widespread, and only a fraction of those infected develop MCC. Key risk factors include:
- UV Exposure: Chronic, unprotected sun exposure or tanning bed use damages DNA.
- Age: The average diagnosis age is 74.
- Weakened Immune System: Conditions like HIV or immunosuppressive drugs increase risk.
- Light Skin: Though MCC can affect anyone, it’s more common in lighter skin tones.
- Previous Skin Cancer: A history of skin cancer raises risk.
Diagnosis and Staging
If you notice a rapidly growing skin lesion, immediate medical attention is vital. Diagnosis involves a physical exam and, critically, a skin biopsy to confirm cancer cells under a microscope.
Staging determines the extent of the cancer’s spread, using the TNM system:
- T: Tumor size and location.
- N: Lymph node involvement.
- M: Metastasis to distant sites.
Stages range from 0 (confined to skin surface) to 4 (widespread metastasis). Accurate staging guides treatment decisions.
Treatment Options
Treatment depends on the stage and spread of the cancer:
- Localized MCC: Surgical excision (wide removal of cancer and surrounding tissue) or Mohs surgery (layer-by-layer removal) are effective. Radiation therapy may supplement surgery.
- Lymph Node Involvement: Surgical removal of affected lymph nodes is necessary.
- Metastatic MCC: Immunotherapy, particularly checkpoint inhibitors (avelumab, ipilimumab, nivolumab, pembrolizumab), shows promise in activating the immune system to fight cancer. Chemotherapy is typically reserved for cases where other treatments fail.
Emerging Therapies: Researchers are exploring oncolytic virus therapy, hormone-like therapies, and targeted treatments. Clinical trials offer access to cutting-edge options.
Prevention and Long-Term Management
Prevention focuses on minimizing risk factors:
- UV Protection: Hats, clothing, broad-spectrum sunscreen (SPF 30+) applied frequently.
- Regular Skin Exams: Monthly self-exams and annual dermatologist visits.
- Post-Treatment Monitoring: Frequent follow-up appointments after treatment to detect recurrence.
The five-year survival rate varies with stage: 79% for localized, 66% for regional, and 31% for metastatic MCC. However, new treatments are improving outcomes.
Conclusion: Merkel cell carcinoma is a serious but treatable cancer when detected early. Vigilance, prompt medical attention, and adherence to treatment protocols are crucial for improving survival rates. Continued research and increased awareness will further enhance outcomes for those affected by this aggressive disease.